Exploring the use of Ultrasound in ALS Training
On the 17th July, Darent Valley Hospital hosted and piloted the first Cardiac Arrest Ultrasound Course in the UK. The course, which is intended as an adjunct to current Advanced Life Support (ALS) training, has been designed to determine when and how ultrasound should be employed within current ALS guidelines and protocols in treating the cardiac arrest patient. Organised and facilitated by Mr. Rob Morrison, Resuscitation Officer at Darent Valley Hospital, attendees comprised critical care nurses and advanced paramedics from London Ambulance Service (LAS).
It has long been acknowledged that the use of ultrasound as a diagnostic aid can be central to the direction of treatment in critical care situations. Bedside echocardiography screening in Emergency Departments is now becoming commonplace, but in critical care, resuscitation and paramedic practice, the use of ultrasound is in its infancy. “Since the 2010 ALS Guidelines, which recognized the potential role of ultrasound imaging during ALS, we have seen an increasing amount of literature relating to the use of ultrasound in resuscitation practice,” said Mr. Morrison.
Until recently, Darent Valley Hospital and London Ambulance Service could not routinely utilize this technology in their clinical management of cardiac arrests. Typically accessible to the larger teaching hospitals, smaller District General Hospitals rarely could provide this option during cardiac arrest events. The prohibitive high cost of ultrasound equipment in these settings has been one of the principal reasons for this, but with the introduction of small and portable ultrasound scanning devices such as the Vscan from GE Healthcare, transthoracic echocardiography is now accessible to a growing number of healthcare disciplines and is now of interest in the fields of resuscitation and paramedic practice. The challenge that remains is the process of training staff to acquire accurate imaging in order to interpret and implement appropriate treatment in accordance with image findings. Darent Valley Hospital’s new course has been designed specifically to meet these training needs.
Incorporating ultrasound in ALS training
While sharing some similarities in content with the UK Resuscitation Council’s Focused Echocardiography in Emergency Life Support (FEEL) course, Mr. Morrison saw a need for a more simplified introductory course as a stepping-stone onto the more advanced training programs. Principally intended to train novice practitioners in the use of TTE during the peri-resuscitation period, the FEEL course is run over one day and followed by on-going study and mentored supervision of 50 scans to be completed within two years. Certification is awarded upon completion by the British Society of Echocardiography (BSE). The Darent Valley introductory course has been designed to concentrate on the use of ultrasound specifically within the management of cardiac arrest events. Commenting on the available sonography expertise at cardiac arrests both within the pre-hospital and District General settings, Mr. Morrison observed, “The number of participants successfully completing the FEEL course is small when compared to the number completing the Resuscitation Council (UK) Advanced Life Support course. We hope our training program will open up the possibilities of providing ultrasound as standard ALS practice for suitable cardiac arrest patients in both general hospitals and pre-hospital environments.”
Getting ‘hands-on!’
Studies have suggested that the pulse check within the ALS algorithm is not a reliable way of detecting the presence or absence of circulation. As the absence of a palpable pulse does not always reflect cardiac standstill during cardiac resuscitation due to possible inefficient cardiac contractions that may occur for a variety of factors, Mr Morrison points out, “If ultrasound can be combined with other techniques such as waveform capnography, we will have an accurate way of quickly assessing the effectiveness of a patient’s circulation without the need for unreliable pulse checks or invasive techniques such as arterial lines.” The course covered the basics of ultrasound including: practical sessions focusing on how to use the Vscan; correct probe handling and views; compliancy with ALS guidelines; human factors and teamwork within an emergency simulated scenario and a subsequent debrief.
Using a combination of real volunteers and the hospital’s new HeartWorks TTE Mobile simulator, the emphasis of the day was to get all delegates ‘hands-on’. Mr. Robert Sargent, Cardiac Physiologist at the hospital first demonstrated the principles of ultrasound practice and using the HeartWorks simulator, showed delegates how to use the probe to obtain the correct views. “One of the main views we focused on was the subcostal view as it is ideal during Cardio Pulmonary Resuscitation (CPR) being away from the area of chest compressions and defibrillation pads,” said Mr. Sargent. “The simulator’s ability to show realistic 3D anatomy of the heart and its internal structures alongside the corresponding ultrasound view obtained with the probe, allowed delegates to really ‘see inside’ and helped them to understand exactly what they were looking at.”
10 seconds and counting!
While the subcostal view is one of the easiest for novice sonographers to learn, it is also one of the most useful to examine all four cardiac chambers and the pericardium. To be able to perform a scan in an ALS compliant way required delegates to be given the time to practice extensively both on the simulator and volunteers using the Vscan. In an active resuscitation attempt, speed is paramount. The scan is performed as part of the ‘non-shockable’ limb of the ALS algorithm during the brief interruption for rhythm assessment so as not to adversely impact upon performance of high quality CPR. Once delegates were sufficiently competent in locating the heart and performing a scan, the course moved onto putting these skills into effect during a pressurized simulated patient scenario.
Delegates were put into cardiac arrest teams and made to perform scans under pressure and without interrupting the ALS protocol. At the end of the two-minute cycle of CPR, a team member counted out the 10 seconds for rhythm /output assessment during which time another member of the team immediately performed a subcostal scan either on a volunteer or the simulator. Whatever the image obtained, at the end of the countdown CPR was restarted. While CPR continued, the team reviewed the recorded images, in particular, to determine whether the patient was presenting Pulseless Electrical Activity (PEA) and to distinguish which type (Normotensive PEA, Pseudo-PEA or True-PEA).
The discussion of PEA and implications for patient presentations in resuscitation attempts was a key topic of interest in the course as employing ultrasound with waveform capnography can help to prognosticate likely outcomes and minimise interventions that might be harmful or of no benefit to patients with PEA. London Ambulance Service has recently trained twelve of its Advanced Paramedics in the use of ultrasound having recently acquired a number of portable Vscan devices. Similarly, at Darent Valley Hospital, the Vscan is taken to every cardiac arrest call.
Addressing the wider interest in echo at a District General Hospital
Darent Valley Hospital is now seeking to address a growing and wider interest in echocardiography training partly due to the Vscan providing greater accessibility to ultrasound along the patient care pathway. The HeartWorks TTE Mobile simulator is now allowing the hospital to produce unique and challenging cardiology and medical scenarios, as well as providing a fixture in the training room for staff who do not routinely practice ultrasound within their clinical disciplines to be able to refine and keep these newly acquired skills current.
“Candidate evaluations from this first pilot course have been excellent,” said Mr. Morrison. “We will look to make improvements and develop it further with the new 2015 Resuscitation Council (UK) Guidelines and maintain a close partnership with LAS to ensure the course is truly multidisciplinary. It is hoped that a limited number of external places will now be available to our local colleagues.”
For course enquiries please email: rob.morrison@nhs.net
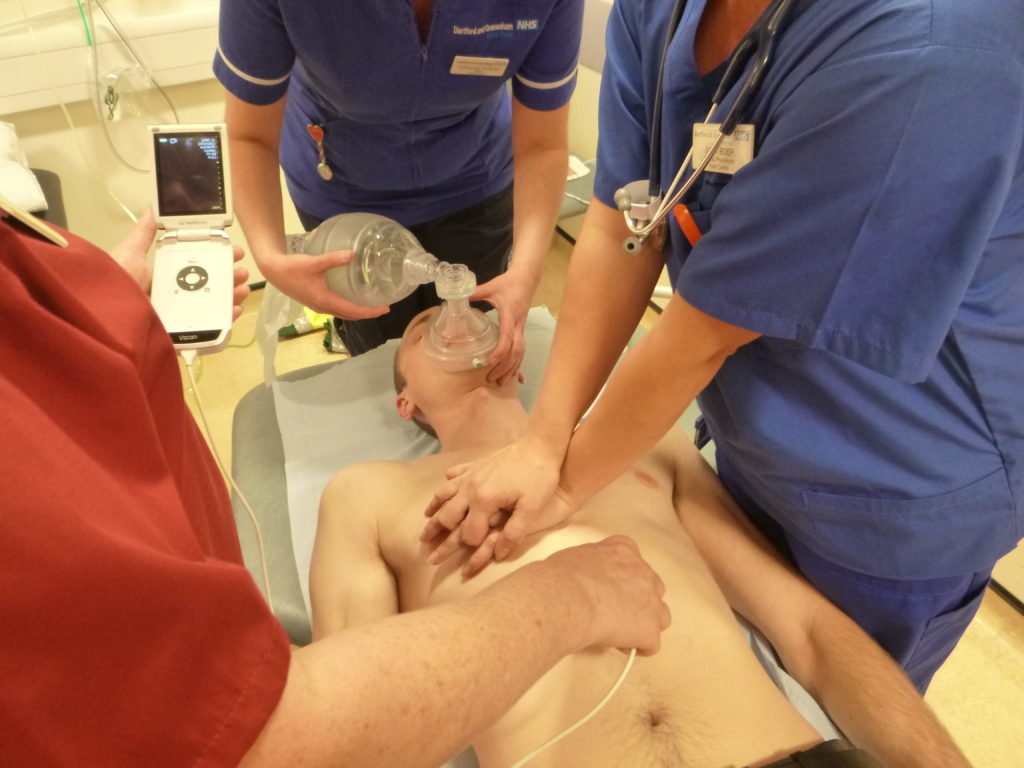
One of the main views we focused on was the subcostal view as it is ideal during CPR being away from the area of chest compressions and defibrillation pads.
Mr. Rob Morrison, Resuscitation Officer at Darent Valley Hospital